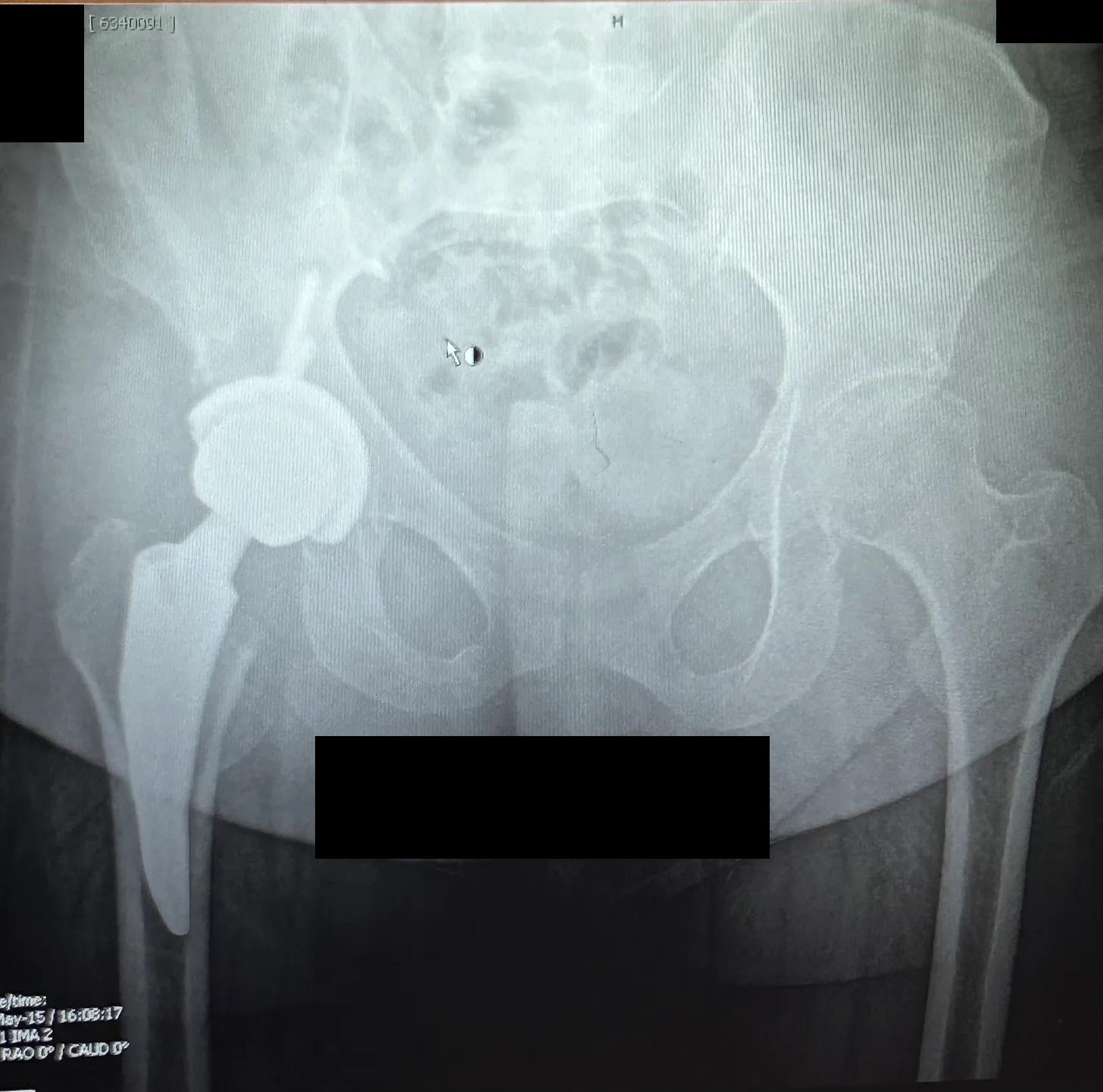
It’s been one year since my hip replacement.
Time is a weird, fluid thing. It feels like it’s only been a few months since surgery, but at the same time my body can tell it’s been longer because I’m walking better than pre-surgery and I “graduated” from physical therapy (PT). Really — they gave me a certificate and everything!
Minutes after waking up from surgery
Apparently, I was very inappropriate while the anesthesia wore off. That stuff is no joke. The nurse who was wheeling me out of the operating room told me he was taking me to room 2. That made me think of the Violent Femmes’ “Kiss Off”, which I began to sing to him. “I take one, one, one cause you left me, and two, two, two for my family …”.
That wouldn’t have been so bad, but then I thought of the Violent Femmes’ “Blister In the Sun”, which, I proceeded to explain to the nurse, was about masturbation. I probably sang the lines, “Big hands, I know you’re the one. Body and beats, I stain my sheets, I don’t even know why.” Apparently, the song isn’t even about the solo act, lead singer Gordon Gano clarified in an interview.
Moral of the story … anesthesia is wild.
A week after surgery
I stayed in the hospital for a week after surgery, because where I get treatment, Nemours Children’s Hospital, is technically a children’s hospital (though they recently extended treatment to 35-year-olds with skeletal dysplasia — I just got in under the wire!). It took years to find a doctor, let alone an entire program, who specialized in rare skeletal dysplasias. But that’s another story.

“Regular” (older) hip replacement patients either stay in the hospital for one-two days or leave the same day as surgery. I can’t imagine being pushed out of the hospital immediately after having your hip ripped out of you. Barely able to walk, and sent home. Maybe an at-home physical therapist comes to your house every week, but you don’t have the facility, the machines, the level of care you receive when you’re in-patient.
I’m grateful I had insurance that covered (part of) my surgery and hospital stay, and short-term disability to provide a third of my paycheck (pretty meager, but still something) while I wasn’t working. Though, insurance tried to give me a last minute heart attack mere daysbefore surgery — sending me a letter denying coverage. The nurse practitioner explained that this often happens (yay, healthcare in America) and would likely be resolved. Thank goodness it was.
Nemours has excellent in-facility PT and occupational therapy (OT). During that first week, I did PT/OT twice a day. Relearned how to take the stairs, dragging my wound VAC with me. There’s a special way to take the stairs when recovering from a hip replacement. Going up: first put your left foot (good hip) up on the first step, hold the railing tightly, then lift your right foot (bad/new hip) up on the step where your left foot is. Going down: first hold the railing tightly, put your right foot down on the top step, then follow with your left foot on the same step. Needless to say, a flight takes a long time. It gets quicker over months of recovery.
Right after surgery, the most painful part wasn’t actually my hip but the terrible nerve pain in my right foot. I’d groan and cry from the pain and swelling. The nurses or my partner Faith tried to elevate my foot just so with towels or blankets. They put a continuous supply of heating and ice packs on my foot, thigh, and hip. I’m sure I drove them mad — I was grumpy with pain, definitely not my best self.
The start of my sciatica
My doctors said the surgery could have exacerbated my sciatica from years ago. They were messing around in my body, cutting out my hip joint, and implanting an artificial one, so it’s very likely my nerves were stretched or irritated.
Nearly a decade ago, I injured my back by hunching over my laptop while covering a conference for a newspaper story at the Walter E. Washington Convention Center. At 4’6”, my feet don’t reach the floor in those uncomfortable interlocking convention center chairs, they dangle. Maybe that or furiously typing in a very non-ergonomic position sparked the sciatic fire.

When the session ended, I closed my laptop, slid it into my rolling bag, and got up — or tried to. I wasn’t able to stand up straight. I was having spasms of sharp pain in the lower left side of my back. Numbness spread from my right butt cheek, down my leg, to the arch of my right foot — the classic pins and needles feeling.
Somehow, I inched my way to a bathroom, called my boss, and told him I wouldn’t be able to finish the story. That was the most important thing in my mind. Did I go straight home or to the doctor? No. I (stupidly, stubbornly, all kinds of “s” words-ly) tiptoed over to a seating area and conducted another interview with two sources, asking questions, typing away as they responded like a pro. I’d scheduled the interview in advance, and worried about canceling. They probably had no idea I was in some of the worst pain of my life.
Then, and only then, did I TAKE THE METRO HOME (instead of calling a cab or an ambulance, like I probably should have), wincing and sobbing the entire ride. I got to my stop, and somehow managed to drive the short distance to the friend’s house I was crashing at for the night (since her parent’s lived closer to the Green Line). My stepmom came to pick me up and take me to an emergency physical therapy consult.
That’s when the sciatica started. And when I (my body made me) quit journalism (well, at least daily deadlines; I still write freelance articles).
I went to pain doctors, my orthopedic specialists, a neurologist. They took X-ray after X-ray and an MRI. But nothing showed up on the scans — not a herniated disc, not a bulging disc, not nerve impingement. It’s incredibly frustrating when you’re in excruciating pain and no doctor can tell you why, when your body is a mystery.
The neurologist sent me for a nerve conduction study, where the doctor placed electrode patches on my right leg. The test delivers a mild electric shock to stimulate the nerves and measure how fast and effectively electrical signals travel through them. It can identify nerve damage (including severity and exact location), dysfunction, or muscle disorders. Before he turned the machine on to deliver the minor shock, he warned me. As he kept turning it up, I asked, “did you start?” Afterwards, he told me that the men he tests often cry and scream and the women have much higher pain tolerances. While this was affirming, the results were inconclusive. I didn’t have nerve damage (a very good thing), but still didn’t have any answers for my sciatica pain. The doctor told me that the numbness could go away in a month, in a few years, or never. Such a helpful range.
I tried three cortisone injections in my back. While some people find these helpful, they didn’t alleviate my pain. For the first few days after receiving the injections, they actually increased pain because they can add inflammation and pressure.
Eventually, over many years, the pain and numbness waned. But if I stand for too long (a half hour, sometimes less), or am active several days in a row, or if my foot dangles off the couch, or if I have to make a long drive, the numbness in my foot comes back and my back pain starts up.
Getting home from the hospital
Driving home from the hospital after surgery is always painful, even if you’re drugged up. You’re uncomfortable, you’re weak and can’t reposition yourself very well, you’re grouchy and want to be in bed.
We live two- to three-hours away from the hospital, so after the drive, I was exhausted but still had to do several flights of stairs to get into bed. There was one set of stairs up from the sidewalk to the gate of the D.C. rowhouse I was living in, then from the gate up to the front door, and then from the main level to my bedroom. I don’t know how long it took me to get up all those stairs, but I know it was draining.
3 months post-surgery
The first 3 months or so after surgery were pretty rough because of the nerve pain in my right foot. It set me back in recovery. Made it hard to rest. Made it hard to exercise, which is what I needed to do to get the muscles moving again after not having used them for a good year because of pain. Hip replacement patients tend to be older individuals, whose post-surgery goals might be being able to walk from their bedroom to their kitchen. I had bigger goals of getting back to my activity level — or beyond — pre-surgery.

I tried heel lifts all throughout the day and night, when I’d wake up once my pain meds wore off. My partner or sister would fill a small basin with Epsom salt and hot water, and I’d soak my right foot until the water cooled. I was very lucky that they massaged my foot every so often — it made such a difference.
For the first few sessions of PT, I needed to use a wheelchair. I didn’t have energy to use a walker for even short distances. The pain would flare and I was hobbling around due to the 9-inch wound healing along my hip and thigh.
After a week or two, I moved from the wheelchair to a walker. Eventually I was able to use a four-pronged cane. Then a single-point cane. And then, somehow, nothing but my own two feet.
I really appreciate my physical therapist, Alice, who made coming to the office fun and motivating. I saw quite a few therapists at the rehab center over the course of nearly two years — one year pre-surgery, to strengthen my body as much as possible, and nearly a year post-surgery — and they all made recovery a little more enjoyable.
I worked on building back my walking and standing stamina. It was hard to walk around the block and stand for 10 minutes. But a few months before that, I wasn’t able to walk or stand much at all. My physical therapist said my strength would improve each week. I was rebuilding all the muscles a hip uses — abductors, adductors, glutes, iliopsoases, lateral rotator muscles. I needed to try to be more patient with my body, while also looking forward to less restrictions.
4-6 months after surgery

Four months after surgery, I went to the beach with my partner and her family. Walking across the sand felt like climbing a mountain, each little grainy ripple my own Sisyphean hill. Carrying bags and a beach chair winded me — I had to take several breaks to even get to the shoreline. After trying the first trek cane-less, I brought my cane the next times we went down to the water, which made it a little easier to walk across the sand. Canes do assist with balance, that’s what they’re for.
As the summer turned to fall and winter again, I noticed I was able to feel the implant in my thigh more when the temperature dropped or when it rained. Sometimes it’s painful, mostly just eerie.
Six months post-op, I had an X-ray taken to check on my implant. The doctors wanted to see if it was still positioned correctly. It grossed me out to think about something inside me that could move out of place. Thankfully, they said it looked perfect — and hopefully it stays that way.
Today
A year post-surgery, my gait is much better, my hip-related pain is vastly reduced, and my walking and standing stamina has improved. I can climb flights of stairs fairly well, if I do say so myself. I’m able to walk through a grocery store, commute to and from work, walk the dog with Faith, go clothes shopping, even wander around airports and Kraków, Poland with family. (Another story delving further into that trip, soon).
I’m not completely without pain. The intensity of the numbness — a weird oxymoronic paradox of my body — has dialed down like turning a volume knob. But it’s still humming. When my back pain creeps up and the bottom of my right foot tingles, I need to sit down to alleviate the pressure and regain feeling in my foot. The numbness is a reminder to listen to my body, to rest — which is hard, since I want to do so many things with my new hip. But rest and recovery is essential. Why is it so hard to remember this, even as someone who’s had chronic pain since childhood?
Will this numbness ever go away completely? Nobody knows — that’s the scary truth. Not the doctors. Not my physical therapist. Not my X-rays. Not my improved gait. Not even me, who lives in my own damn body where the pain is actually happening. That’s the thing about recovery. It’s an ongoing, kind of forever process. You never stop recovering — your body is continuously healing and regenerating, becoming inflamed, getting injured, experiencing life and little traumas every day.



My right hip will always be artificial. As one of my orthopedic surgeons said, “never as good as the man upstairs can make.” My body — muscles, nerves, posture, everything — is relearning how to have a workable hip, how to walk and do activities without a failing, deteriorating hip joint. So, this is the first boulder to cross the river. The river is wide, the current swift, the boulders spread way out. But — I’ve crossed the first one, made it to the other side of surgery. Recovered, and am still recovering.
I’m so grateful to have this new hip and for every person who helped me get here: my love, Faith, my sister, my mom and stepdad, my dad and stepmom, family who visited me in the hospital, my surgeons and doctors, my nurses, my physical therapists, the therapy dogs that visited me in the hospital and my own dog and cat, and everyone else I failed to mention.
Thanks for reading about my recovery journey. I know that this is just the beginning. I’m hoping to have many, many pain-free (or as close to pain-free) years with my new hip. Until I’ll inevitably need to replace my left hip or have a second hip replacement on my right hip. Artificial hips are lasting a lot longer these days, but they still don’t last forever. And since I’m young, it’s likely to wear out quickly. But that’s for the future. For now, cheers to getting hip!


